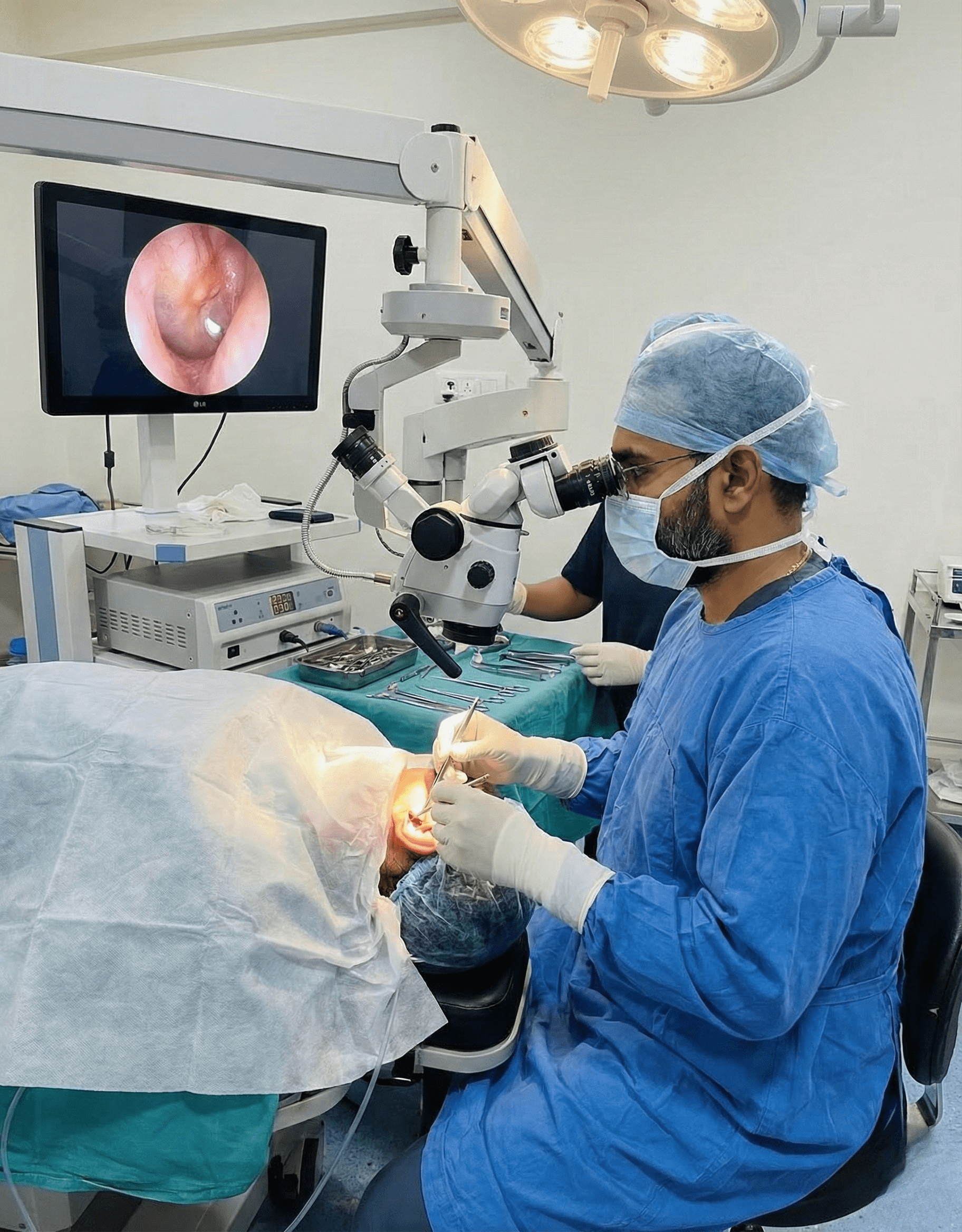
Tympanoplasty is a surgical procedure performed to repair a perforated or damaged eardrum (tympanic membrane) and restore normal hearing function. A healthy eardrum plays a vital role in sound transmission and protects the middle ear from infections. When an eardrum perforation is left untreated, it can result in recurrent ear infections, persistent ear discharge, and progressive hearing loss. At our ENT hospital, tympanoplasty is performed using advanced microscopic and endoscopic techniques to ensure high precision, safety, and durable hearing improvement.
Tympanoplasty is usually recommended for patients experiencing chronic ear discharge that does not respond to medication, hearing loss caused by eardrum perforation, recurrent middle ear infections, or eardrum damage due to trauma or infection. It may also be advised when the eardrum fails to heal on its own over time. Before recommending surgery, our ENT specialists conduct a thorough clinical evaluation along with detailed hearing assessments to determine the most appropriate and effective treatment plan for each patient.
After tympanoplasty, patients are guided with clear post-operative instructions, medication support, and follow-up visits. Most patients experience gradual hearing improvement within a few weeks. Our team ensures continuous monitoring for safe healing and optimal outcomes.
We follow a patient-centric and evidence-based approach for every ear surgery. The procedure is performed under sterile, controlled conditions using modern surgical microscopes for enhanced accuracy.
Tympanoplasty is a routine ENT surgical procedure and is considered safe when performed by an experienced ENT surgeon.
The procedure typically takes 1 to 2 hours, depending on the size and location of the eardrum perforation.
Yes, most patients experience significant improvement in hearing after successful healing.
In most cases, tympanoplasty is done as a short-stay or day-care procedure.
Initial recovery takes a few days, while complete healing of the eardrum may take several weeks.
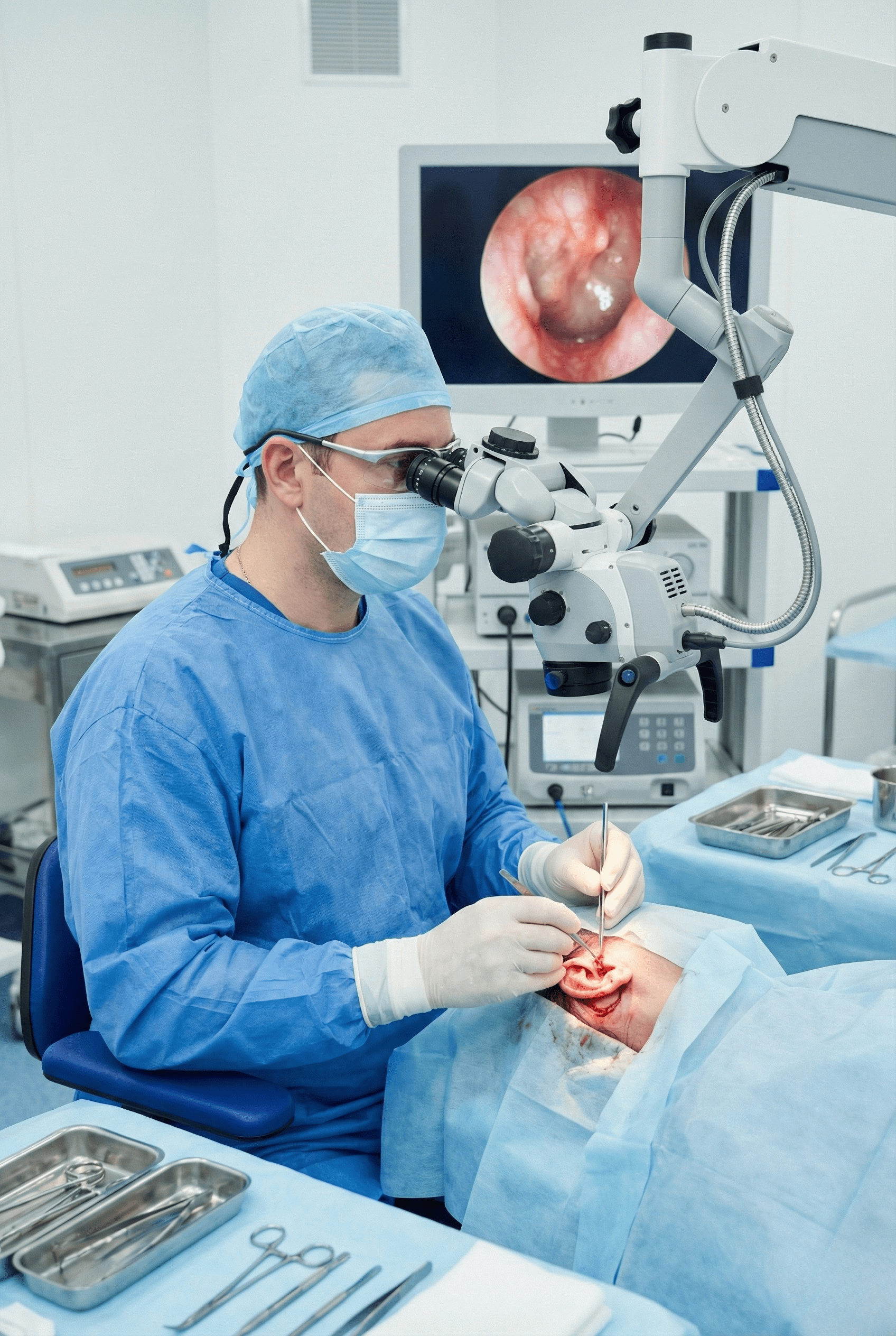
Tympanoplasty with mastoidectomy is a combined ear surgery performed to repair a perforated eardrum and remove chronic infection from the mastoid bone located behind the ear. The mastoid contains air cells that can become infected due to long-standing middle ear disease. If untreated, this condition may lead to persistent ear discharge, hearing loss, dizziness, or serious complications. At our ENT hospital, this surgery is performed using advanced microscopic and endoscopic techniques to completely clear infection while restoring ear structure and hearing function.
This procedure is commonly recommended for patients with chronic suppurative otitis media, cholesteatoma, persistent ear discharge, hearing loss, or mastoid bone involvement seen on imaging. It may also be advised when medical treatment fails to control infection. Before surgery, our ENT specialists conduct a detailed clinical examination, hearing tests, and imaging studies to plan safe and effective treatment.
After surgery, patients receive detailed post-operative guidance, medications, and scheduled follow-ups. Hearing improvement occurs gradually as healing progresses. Our team closely monitors recovery to prevent recurrence and ensure long-term success.
We follow a patient-focused, evidence-based surgical approach using modern operating microscopes and sterile modular operation theaters to ensure precision and safety.
Yes, it is a standard ENT procedure when performed by experienced surgeons.
The procedure usually lasts 2 to 3 hours.
Most patients notice hearing improvement after healing.
Short hospitalization may be advised depending on infection severity.
Complete healing may take several weeks.
Revision mastoidectomy is a corrective ear surgery performed when infection or disease persists or recurs after a previous mastoid surgery. Residual cholesteatoma, recurrent infection, or incomplete clearance can cause ongoing ear discharge, hearing loss, and discomfort. This procedure focuses on removing remaining disease tissue while preserving healthy ear structures. At our ENT hospital, revision mastoidectomy is performed with high-precision microscopic techniques to ensure complete disease clearance.
This surgery is recommended for patients with continued symptoms after earlier ear surgery, recurrent infections, hearing deterioration, or imaging evidence of residual disease. A detailed ear examination, hearing evaluation, and imaging studies are essential before planning revision surgery to achieve optimal outcomes.
Post-operative care includes medication, wound care instructions, and regular follow-ups. Recovery is gradual, and hearing improvement depends on disease severity and reconstruction performed.
We prioritize meticulous surgical planning, advanced visualization, and careful tissue handling to minimize recurrence and protect hearing.
Due to persistent or recurrent ear disease.
Yes, it requires expert surgical skill.
Most patients experience symptom relief.
Short stay may be advised.
Healing usually takes a few weeks.

Myringotomy with grommet insertion is a minor surgical procedure performed to create a small opening in the eardrum and place a tiny ventilation tube (grommet) to allow air to enter the middle ear. This procedure helps equalize ear pressure and prevents the buildup of fluid behind the eardrum. Persistent middle ear fluid can interfere with hearing and speech development, especially in children, and may increase the risk of repeated infections. At our ENT hospital, this procedure is carried out using precise microscopic techniques to ensure safety, accuracy, and long-term relief from ear-related problems.
Myringotomy with grommet insertion is usually recommended for patients suffering from recurrent ear infections, persistent fluid in the middle ear, hearing loss due to fluid accumulation, or frequent ear pain caused by pressure imbalance. It is commonly advised for children with glue ear but may also be recommended for adults with chronic middle ear issues. Before suggesting surgery, our ENT specialists perform a detailed ear examination along with hearing tests to confirm the necessity and suitability of the procedure.
After the procedure, patients receive detailed aftercare instructions, medications if required, and scheduled follow-up visits. Hearing improvement is often noticed soon after surgery. Our team closely monitors recovery to ensure proper tube function and healing.
We follow a gentle, patient-focused, and evidence-based approach for this procedure. Surgery is performed in a sterile environment using advanced microscopes to achieve precise tube placement with minimal discomfort.
The procedure is usually performed under anesthesia and is not painful during surgery.
Grommets typically remain in place for 6 to 12 months and fall out naturally.
Certain precautions may be advised, especially during bathing or swimming.
Many patients notice hearing improvement soon after fluid drainage.
Yes, it is a commonly performed and safe ENT procedure in children.
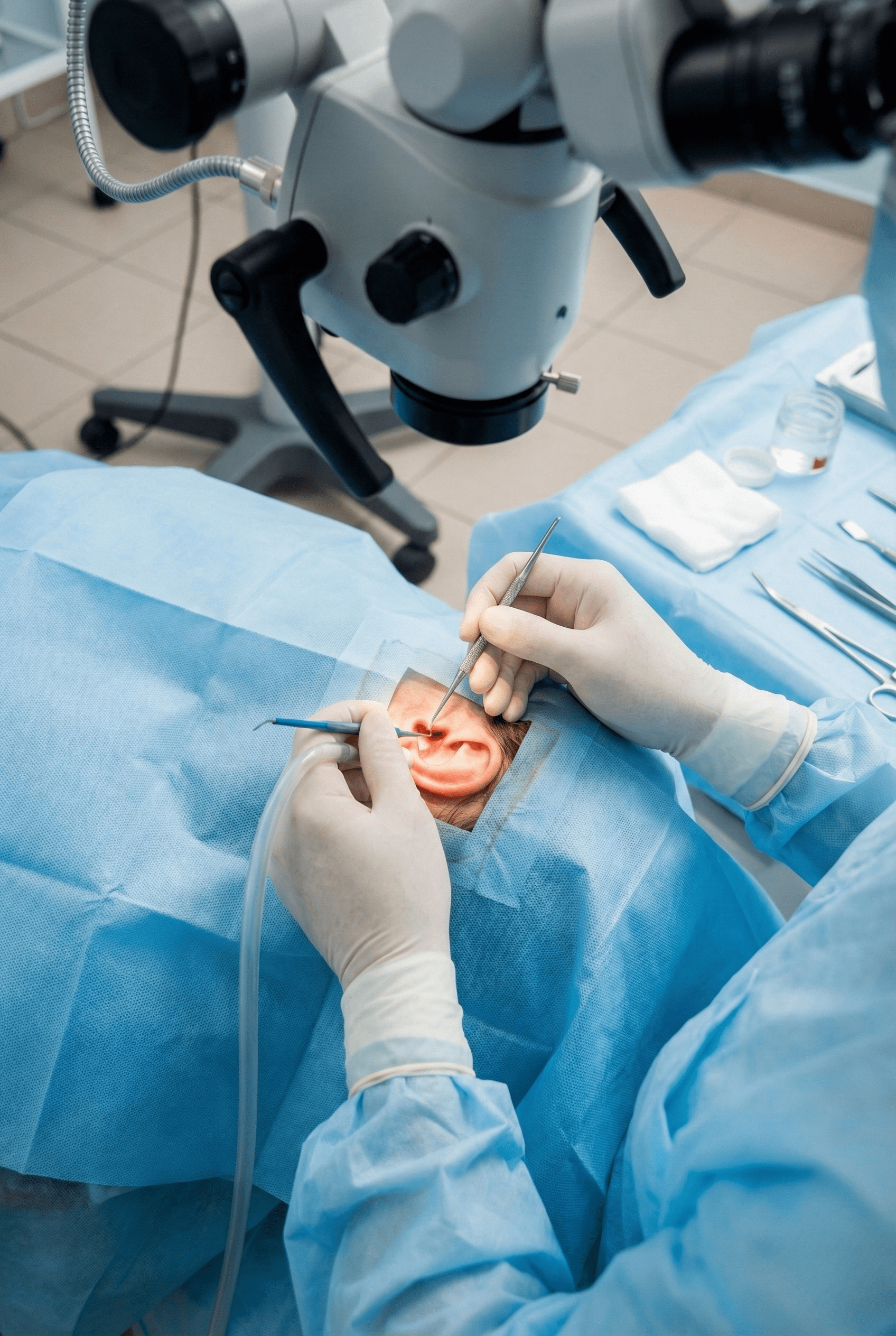
Stapedectomy or stapedotomy is a specialized ear surgery performed to treat hearing loss caused by otosclerosis, a condition where the stapes bone in the middle ear becomes fixed and prevents sound vibrations from reaching the inner ear. This procedure involves removing or modifying the affected stapes bone and replacing it with a prosthetic device to restore sound transmission. If left untreated, otosclerosis can lead to progressive hearing loss over time. At our ENT hospital, stapedectomy and stapedotomy are performed using advanced microscopic techniques to ensure precise correction and long-term hearing improvement.
This surgery is recommended for patients experiencing gradual hearing loss due to otosclerosis, difficulty hearing conversations, or poor hearing despite medical treatment or hearing aids. A comprehensive ENT evaluation, hearing tests, and imaging studies are performed before recommending surgery to confirm diagnosis and suitability for the procedure.
After surgery, patients are provided with clear post-operative instructions, medications, and follow-up schedules. Hearing improvement usually develops gradually as healing progresses. Regular monitoring ensures safe recovery and optimal results.
We adopt a meticulous, patient-centric approach using high-magnification surgical microscopes and proven techniques. Each surgery is carefully planned to maximize hearing restoration while minimizing risks.
It is a well-established ENT procedure when performed by an experienced surgeon.
The procedure usually takes about 1 to 2 hours.
Hearing typically improves gradually over several weeks.
Usually, only one ear is operated on at a time for safety reasons.
Most patients experience long-lasting hearing improvement after surgery.

Cochlear implant surgery is an advanced hearing restoration procedure designed for individuals with severe to profound sensorineural hearing loss who do not benefit adequately from hearing aids. The surgery involves placing an electronic device that directly stimulates the auditory nerve, allowing sound signals to reach the brain. Without timely intervention, severe hearing loss can significantly impact communication, learning, and quality of life. At our ENT hospital, cochlear implant surgery is performed using modern surgical techniques to ensure precision, safety, and optimal implant performance.
Cochlear implantation is recommended for children and adults with profound hearing loss, delayed speech development due to hearing impairment, or poor speech understanding despite hearing aids. Prior to surgery, patients undergo a detailed evaluation including hearing tests, speech assessments, imaging studies, and counselling to determine candidacy and expected outcomes.
After surgery, patients receive structured post-operative care, wound management, and follow-up visits. Implant activation and speech therapy sessions are scheduled to support gradual hearing adaptation and communication improvement.
We follow a multidisciplinary, patient-centered approach involving ENT surgeons, audiologists, and speech therapists. Surgery is performed in a controlled environment using advanced technology to ensure accurate implant placement.
Yes, it is a well-established and safe procedure when performed by trained specialists.
Hearing improves significantly, but it differs from natural hearing.
The procedure usually lasts 2 to 3 hours.
Yes, speech and auditory therapy play a crucial role in success.
Yes, adults with severe hearing loss can achieve meaningful hearing improvement.
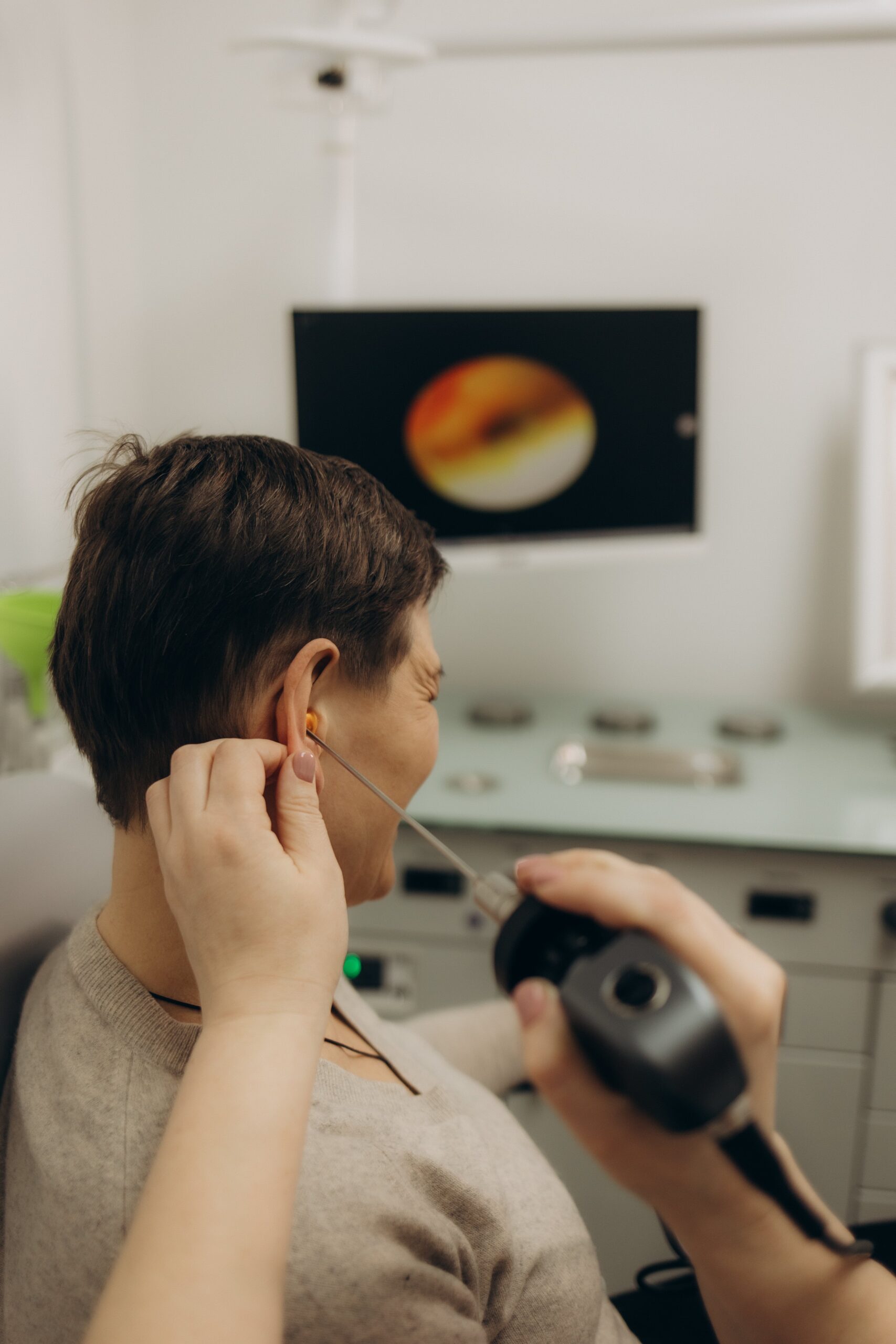
Endoscopic assisted impacted wax removal is a precise ENT procedure performed to safely remove hardened or deeply impacted earwax using an endoscope for enhanced visualization. Excessive or impacted earwax can cause hearing loss, ear pain, tinnitus, dizziness, and recurrent ear infections if not managed properly. Traditional methods may be ineffective or unsafe in such cases. At our ENT hospital, this procedure is carried out using high-definition endoscopic guidance to ensure complete removal while protecting the ear canal and eardrum.
This procedure is recommended for patients experiencing blocked ears, reduced hearing, ear discomfort, ringing sensations, or dizziness caused by impacted wax. It is especially useful for patients with narrow ear canals, previous ear surgeries, or sensitive eardrums. Our ENT specialists perform a detailed ear examination before planning safe and effective wax removal.
The procedure provides immediate relief. Patients can resume normal activities the same day, with minimal aftercare instructions.
We use endoscopic precision, gentle techniques, and sterile instruments to ensure safe, painless, and complete wax clearance.
Yes, it is one of the safest methods due to direct visualization.
No, it is generally painless and well tolerated.
Usually completed within 15–30 minutes.
Yes, some individuals may need periodic cleaning.
No anesthesia is usually required.
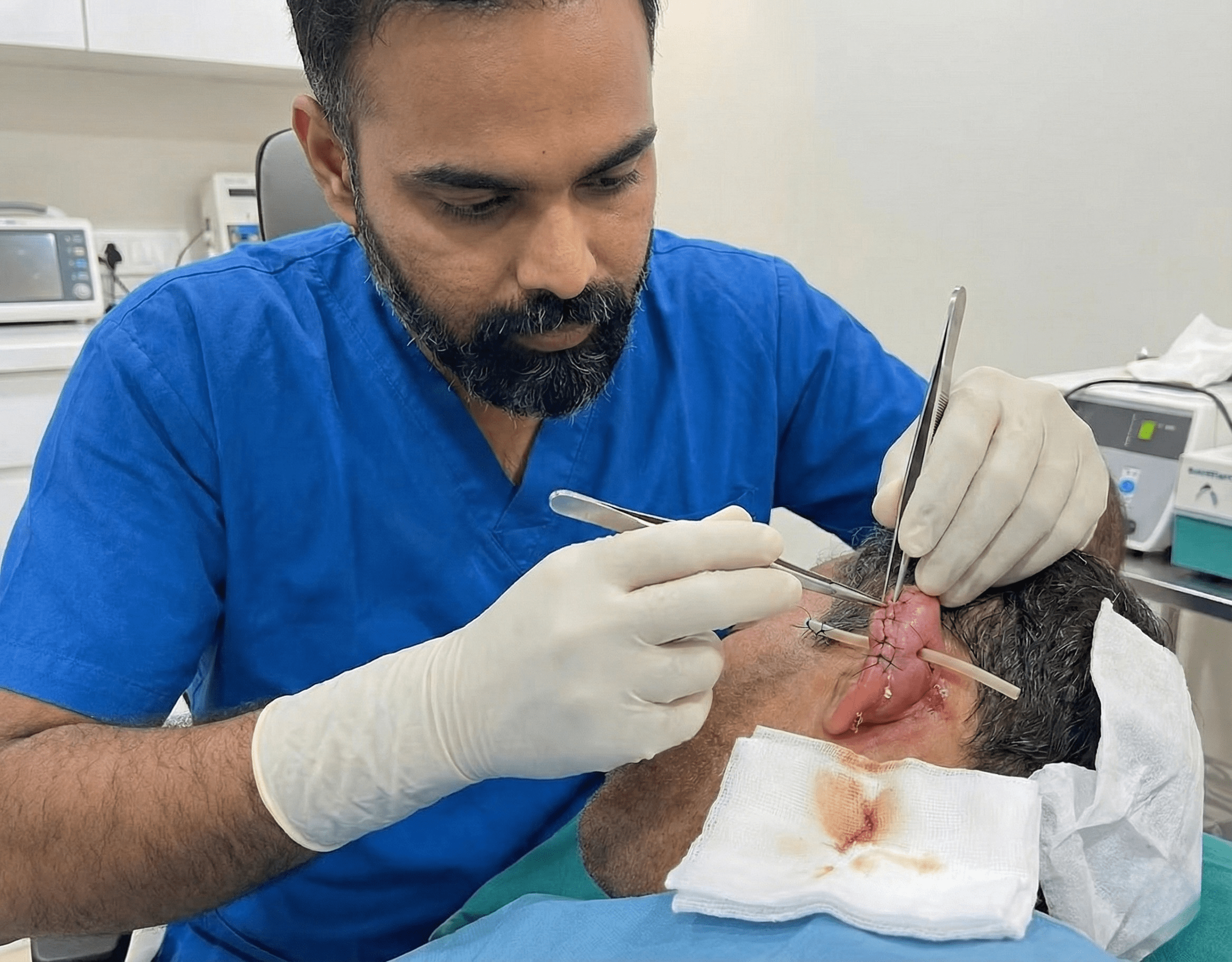
Seroma ear surgical drainage is a procedure performed to remove collected clear fluid (seroma) from the ear, usually following trauma, surgery, or inflammation. If untreated, a seroma can cause pain, swelling, infection, or deformity of the ear structure. Surgical drainage with suturing helps evacuate the fluid, prevent recurrence, and restore the ear’s normal contour. At our ENT hospital, the procedure is performed using sterile techniques for safe and effective outcomes.
This procedure is recommended for patients experiencing ear swelling, discomfort, fluid accumulation, or post-traumatic ear deformity. Early intervention prevents complications such as infection or cartilage damage. Our ENT specialists evaluate the condition thoroughly before planning drainage and repair.
Patients are advised on wound care, medications, and follow-up visits. Healing is usually smooth with noticeable improvement in ear shape and comfort.
We follow a structured, evidence-based approach with precise drainage, proper suturing, and close follow-up to prevent recurrence.
Yes, it is a minor ENT surgical procedure.
Sutures are placed carefully to minimize scarring.
Usually done as an outpatient procedure.
Recurrence is uncommon with proper suturing.
Most patients recover within 1–2 weeks.
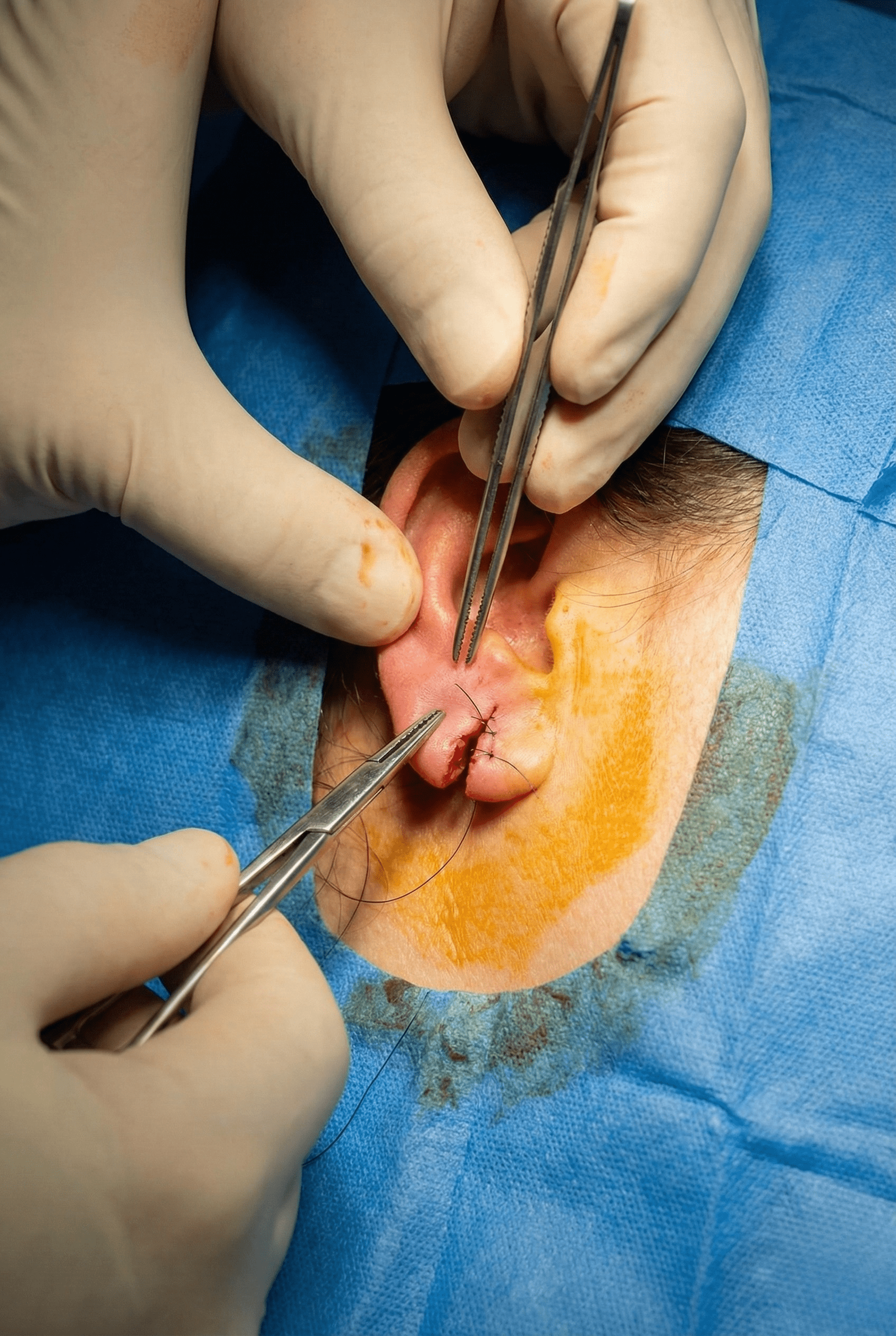
Split ear lobe repair is a minor surgical procedure performed to correct partially or completely torn ear lobes caused by trauma, heavy earrings, or prolonged use of ear ornaments. A split ear lobe can affect appearance and prevent wearing earrings comfortably. At our ENT hospital, ear lobe repair is performed using refined surgical techniques to restore the natural shape and symmetry of the ear lobe with minimal scarring.
This procedure is recommended for individuals with torn, stretched, or damaged ear lobes affecting aesthetics or function. Our ENT specialists assess the extent of the split and plan repair based on ear anatomy and cosmetic considerations to achieve optimal results.
Patients receive clear wound-care instructions and follow-up guidance. Healing is usually quick, and ear piercing can be done later after complete recovery.
We emphasize cosmetic precision, sterile technique, and patient comfort to ensure natural-looking and lasting results.
The procedure is done under local anesthesia for comfort.
Usually completed within 30–45 minutes.
Scarring is minimal when properly cared for.
Yes, after complete healing as advised by the doctor.
Yes, with proper care, results are long-lasting.